In many parts of the world good mental health at work has finally moved from being a ‘nice-to-have’ to a business imperative.
This increased prioritization is not only good for employees, but is also good for employers. Good mental health practices have been found to be a key factor for attracting and retaining talent, increasing productivity, boosting morale and is more important than ever in a changing world. This is important for all generations, especially the upcoming generation of workers. Research released by Mckinsey Health Institute this week has found that nearly one in four Gen Z respondent report their mental health worsening in the past three years in response to regional and global crises, higher than any other generation.
However, the benefits of having mental health policies and plans in place in any workplace only occur if the solutions that are implemented actually work.
So, how do you know if your workplace mental health solutions are working to improve the mental health of your employees?
The WHO Guidelines On Mental Health At Work released today provide a comprehensive overview of evidence-based recommendations on interventions that can be implemented to better prevent, protect and promote, and support the mental health of workers.
These comprehensive guidelines have been developedfollowing a systematic review of evidence worldwide by a wide consortium of experts, let by the World Health Organization, funded by Wellcome.
For those short on time to digest the 100+ pages of the guidelines, a short policy brief has also been released, developed as a joint collaboration between the WHO and the International Labor Organization. This briefing is designed to support various stakeholders fulfill their respective roles and take action, primarily focused on national and workplace policy makers – especially governments, employers and representative organizations.
Two recommendations in the publications stand out a great place to start and guide adaption of solutions for any employer.
Firstly, you should develop a specific policy and plan for mental health at work that aims for continual improvement and is integrated into the Occupational Health and Safety Management system.
While this may seem like an obvious recommendation, it is surprising how many companies don’t have this in place. Only 37% of large companies surveyed in the UK recently by CCLA published the existence of a stand alone mental health policy or plan, and 17% a partial plan.
Many large companies are building the internal resources needed to develop and implement this kind of plan. The increasingly common job openings for ‘Chief Wellbeing Officer’ for large employers demonstrates the shift to having dedicated leadership and resources to mental health as a cross-cutting business priority. However, small and medium enterprises (which account for about 90% of businesses and more than 50% of employment worldwide, according to the World Bank) rarely have the resources available to dedicate to developing a custom plan, especially during times of economic challenge.
The guidelines provide a number of recommendations of key approaches which have been thoughtfully designed to be applicable to all organization sizes and geographies. Importantly, they also pay particular attention to front line workers, including those working in humanitarian and crisis settings around the world.
Particular attention is paid in the guidelines to the importance these policies and plans to:
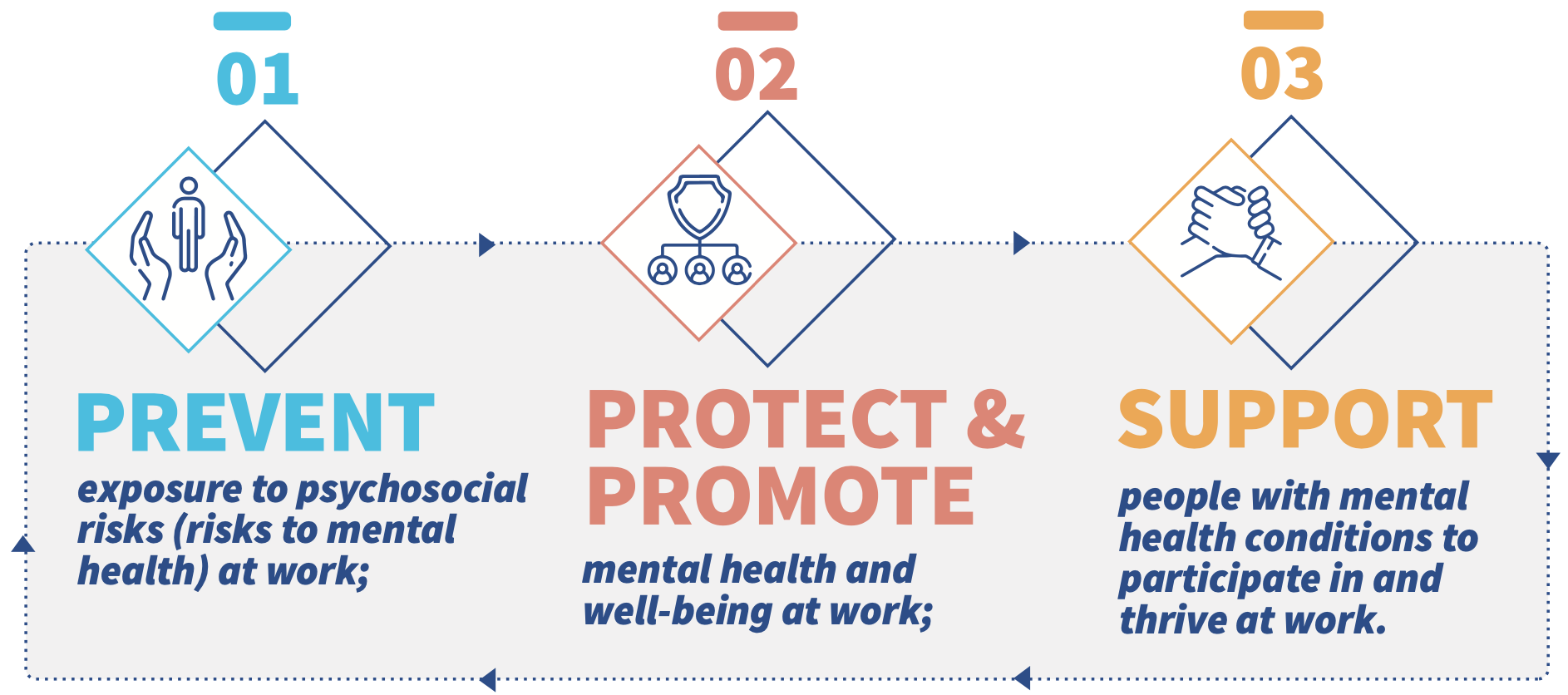
1. Preventing the risks to mental health at work, such as heavy workloads, limited autonomy, inflexible hours, through organizational interventions.
2. Protecting and promoting mental health though training managers – to better support their staff and strengthen interpersonal managerial skills; training workers to reduce stigmatizing attitudes for mental health; and delivering whole of workforce interventions that aim to build workers’ stress management skills.
3. Supporting people living with mental health conditions to participate in work– through reasonable accommodations, return to work programmes following an absence, and supported employment to help gain entry to paid work.
The recommendation that these plans and policies should aim for continuous improvement is an important one. One barrier I often hear leaders citing as a reason to hold back from taking more action is the fear of not being perfect. Yes, it certainly can also be the case that mental health indicators – like the number of people taking mental health sick leave – get ‘worse’ before they get ‘better’, but this can be a sign of progress, especially in environments where stigma has prevented employees speaking openly in the past.
However, when it comes to mental health at work, perfection can be the enemy of the good. A commitment to start, understand the impact you’re having through measuring impact, and make continual improvement is a pragmatic one, and required for progress.
Continual improvement is also important when considering the second high level recommendations: ensure that all interventions are based on the latest evidence available.
The recommendations in the WHO guidelines are based on the best evidence currently available. However, they also highlight the gaps in the evidence that were identified during the development process, and are clear on which recommendations have stronger evidence base than others.
These gaps are unsurprising as mental health as an industry has been systematically underfunded and neglected for a long time.
Wellcome is one funder seeking to change this, and has sought to understand the state of the evidence by undertaking reviews of promising approaches for addressing workplace mental health. Their first commission looked at approaches spanning from reducing excessive sitting to flexible working, and their second review, published alongside the guidelines, looked at approaches spanning from preventing sexual harassmentto arts-based interventions. Despite some evidence to inform the use of the interventions, both commissions found significant gaps in the evidence base. This is especially true in low and middle income countries where the evidence remains limited, if available at all. Evidence in small and medium enterprises was also limited.
So, it’s clear that while the quality and diversity of the evidence needs to improve over time. Employers, working together with experts, can be a part of this progress.
One powerful way employers can contribute to the gaps in the evidence base is to track and report the impact of interventions, and share what has worked for you. This is a powerful way for employers to not only be sure your solutions are working, but also contribute to the growingglobal base of knowledge.
For employers, this also means it’s important to make sure that when designing and implementing your mental health at work policies and plans, these are checked against the latest evidence the guideline provides.
The policy brief also provides a menu of some practical considerations for employers to consider including;
1. Allocating financial and human resources for implementing mental health at work policies and interventions
2. Including mental health services in work benefits packages
3. Implementing policies on equality and non-discrimination throughout the full employment cycle
4. Reducing negative attitudes towards mental health conditions through training and proven anti-stigma interventions such as contact-based strategies
5. Ensuring confidentiality and protection from reprisals to promote voluntary disclosure of mental health issues and facilitate access to support
We hope the guidelines and policy brief will support you to evaluate your own mental health plans, and inspire you to invest further in the mental health of your workforce.
As the guidelines so powerfully say “addressing mental health at work effectively will help prepare for the future of work and a changing world.” And, despite the challenges that do exist this “should not be seen as onerous. Rather, it offers an opportunity for growth and sustainable development”.
And, most importantly, everyone has the right to the highest attainable standard of mental health at work.